What monoclonal antibodies are – and why we need them as well as a vaccine
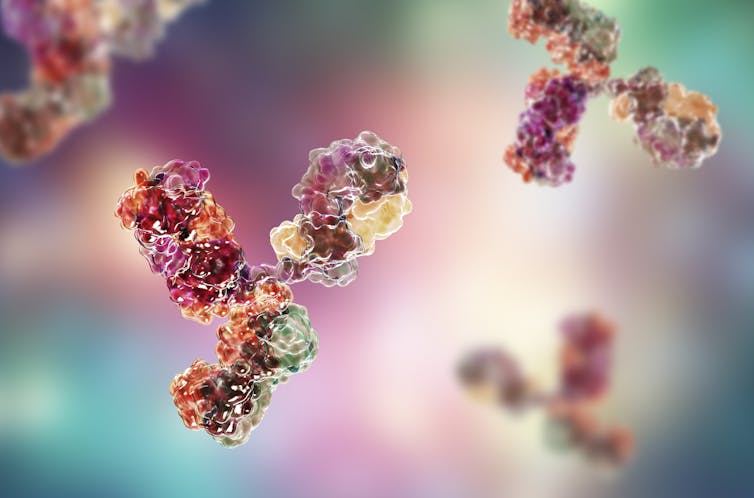
Y-shaped proteins called antibodies are vital for attacking and destroying the virus. Dr_Microbe/Getty Images
Courtesy of Rodney E. Rohde, Texas State University
When President Trump was diagnosed with COVID-19, one of the cutting-edge experimental therapies he received was a mixture of monoclonal antibodies. But now a vaccine may soon be available. So are other therapies necessary or valuable? And what exactly is a monoclonal antibody?
Over the past few months, the public has learned about many treatments being used to combat COVID-19. An antiviral like remdesivir inhibits the virus from replicating in human cells. Convalescent plasma from the blood of donors who have recovered from COVID-19 may contain antibodies that suppress the virus and inflammation. Steroids like dexamethasone may modify and reduce the dangerous inflammatory damage to the lungs, thereby slowing respiratory failure.
The FDA issued emergency use authorization for Eli Lilly’s monoclonal antibody, called bamlanivimab, and Regeneron is waiting for FDA’s green light for its antibody treatment. Monoclonal antibodies are particularly promising in therapy because they can neutralize the SARS-CoV-2 virus, which causes COVID-19, and block its ability to infect a cell. This might be a lifesaving intervention in people who are unable to mount a strong natural immune response to the virus – those over 65 or with existing conditions that make them more vulnerable.
I’ve worked in public health and medical laboratories for decades, specializing in the study of viruses and other microbes. Even when a vaccine for COVID-19 becomes available, I see a role for monoclonal antibody therapy in getting the pandemic under control.
Why should we care?
Until a large percentage of a population has immunity to an infectious disease – either through a vaccine or the unchecked spread through a community – the world must rely on other weapons in our war against the COVID-19 pandemic.
Herd immunity results when the majority of the population gains immunity to the virus either through vaccination or infection. When this happens, vulnerable people who cannot get vaccinated are protected by the ‘herd.’ smodj/iStock/Getty Images Plus
Along with the previously mentioned therapies, monoclonal antibodies can offer us another tool to neutralize the virus once it causes an infection.
These man-made antibodies offer the world the possibility of immunotherapy similar to the use of convalescent plasma but with a more targeted and accurate action. While a vaccine will ultimately help protect the public, vaccination will not be an instantaneous event, delivering vaccine to 100% of the population. Nor do we know how effective it will be.
The impact of a vaccine also isn’t instantaneous. It takes several weeks to generate a powerful antibody response. In the interim, monoclonal antibodies could help mop up virus that is multiplying in the body.
Antibody 101
An antibody is a Y-shaped protein naturally produced by our body’s immune system to target something that is foreign, or not part of you. These foreign bodies are called antigens and can be found on allergens, bacteria and viruses as well as other things like toxins or a transplanted organ.
A monoclonal antibody treatment mimics the body’s natural immune response and targets foreign agents, like a virus, that infect or harm people. There are also monoclonal antibodies that pharmaceutical companies have designed that target cancer cells. Monoclonal antibodies are one of most powerful types of medicine. In 2019 seven of the top 10 best-selling drugs were monoclonal antibodies.
For President Trump, the experimental treatment made by the pharmaceutical company Regeneron included two antibodies.
Typically the spike protein on the coronavirus fits perfectly into the ACE2 receptor on human cells, a protein common in lung cells and other organs. When this connection happens, the virus is able to infect cells and multiply inside them. But monoclonal antibodies can slow or halt the infection by attaching to the viral spike protein before it reaches the ACE2 receptor. If this happens, the virus becomes harmless because it can no longer enter our cells and reproduce.
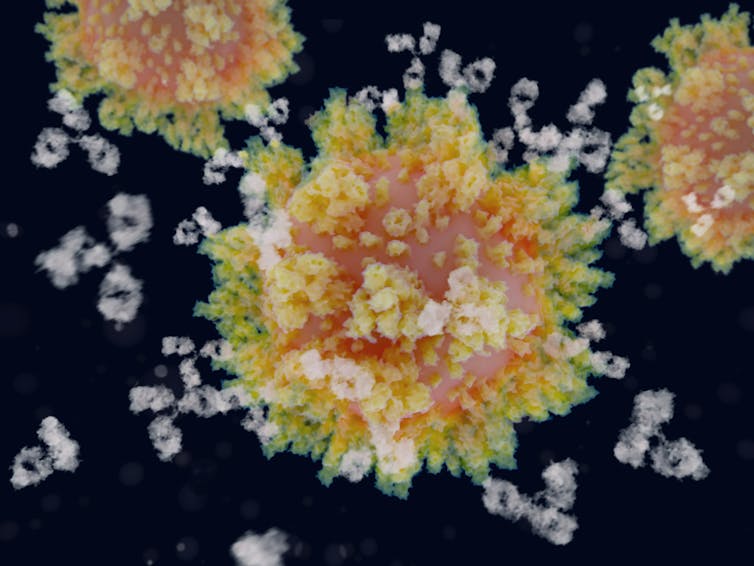
When antibodies (white) bind to the spike proteins covering the surface of the virus, SARS-CoV-2 can no longer infect human cells. JUAN GAERTNER/SCIENCE PHOTO LIBRARY/Getty Images
How are monoclonal antibodies created?
Monoclonal antibodies that neutralize the coronavirus are complicated to manufacture and produce. They must be made inside cells taken from a hamster’s ovary and grown in gigantic steel vats. The antibodies that these cells manufacture must then be extracted and purified. Unfortunately these monoclonal antibodies, which have been used for other illnesses for years, are often quite expensive.
Regeneron’s two antibodies are targeted to the spike protein of SARS-CoV-2 – the protrusions on the surface of virus that give it a crown-like look and are critical for infecting human cells.
One of Regeneron’s two antibodies is a replica, or clone, of an antibody harvested from a person who recovered from COVID-19. The second antibody was identified in a mouse that was biologically engineered to have a human immune system. When this mouse was injected with the spike protein, its human immune system generated antibodies against it. One of the most effective mouse antibodies was then harvested and used to form part of this therapy.
Eli Lilly’s monoclonal antibody therapy, bamlanivimab, was identified from a blood sample taken from one of the first U.S. patients who recovered from COVID-19.
Both companies have in place large-scale manufacturing with robust, global supply chains in place to produce the monoclonal antibodies, with many global manufacturing sites to ramp up supply. Eli Lilly has received FDA approval, and Regeneron is still awaiting approval. Unfortunately, there will likely be a shortage of the antibodies in the early going of approvals.
Monoclonal antibodies plus a vaccine
Monoclonal antibodies will be able to complement vaccines by offering rapid protection against infection. When they are given to an individual, monoclonal antibodies provide instantaneous protection for weeks to months. Vaccines take longer to provide protection since they must challenge the immune system. But the advantage of a vaccine is that they usually provide long-term protection.
Regeneron’s and Eli Lilly’s products are both delivered by intravenous injection, after which the patient must be monitored by health care professionals. Since they offer immediate protection, the implications to treat or provide protection to high-risk populations is immense.
These medicines have the potential to treat infected patients or prevent infection of essential health care and public health professionals on the front line of this pandemic. Monoclonal antibodies could also be useful for older people, young children and immunocompromised people for whom vaccines either don’t work or can be dangerous.![]()
Rodney E. Rohde, Professor Clinical Laboratory Science, Texas State University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
[Deep knowledge, daily. Sign up for The Conversation’s newsletter.]